
Hypoxia Studies (also coming to Southwestern University!)
Exposure to sustained hypoxic (low oxygen) conditions, arising from a life-threatening injury, illness, surgery, or a trip to the mountains, evokes a rapid increase in ventilation (breathing) that may last from minutes to months, depending on the extent of the hypoxic event. While the central nervous system (brain and spinal cord) is integral to this process, the molecular and physiological mechanisms of ventilatory control are not entirely understood. Understanding how the brain interprets and responds to hypoxic respiratory signals has relevance to many disease states (e.g. COPD and sleep apnea) as well as helping us better understand the mechanisms behind ventilatory acclimatization to hypoxia (VAH), or your body’s continued enhanced ventilation even after the hypoxic signal is gone.

Currently, we are focusing on imaging respiratory control regions of the brain to better understand how changes in ventilation are centrally regulated by both neuronal and non-neuronal cells.
Cellular communication in the brain is not limited to neurons. Astrocytes and microglia are present in respiratory regions of the brainstem and surround neural synapses and neighboring blood vessels, modulating communication of the neural pathways. Astrocytes are a heterogeneous population with cell types that regulate neurotransmitter availability in the synapse and others that are chemosensitive, meaning that they can respond to changes in blood pH. Microglia are thought to be upstream of astrocytes in that upon activation by neurotransmitters released by neurons, microglia release their own gliotransmitters, activating neighboring astrocytes which then amplify neuronal signaling.
In respiratory centers of the brainstem, both microglia and astrocytes are activated as shown by immunofluorescent labeling, and my lab is interested in uncovering the role of these glial cells in respiratory control.

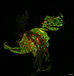
Figure 3: Microglia and astrocytes in the NTS during normoixa and after 24 hours of hypoxia.
Astrocyte activation can be quantitatively studied by immunofluorescent labeling of these cells using a specific antibody, GFAP. When astrocytes are activated they produce more GFAP protein, which translates to a “brighter” more intense signal in an image. Thus, we can calculate the average intensity over baseline (normoxic animals) to get an output of astrocyte “activation”. On the other hand, microglia can be visualized with the Iba-1 antibody and assessed for a morphology shift to the larger “active state”, with more amoeboid-shaped cell bodies. This also requires immunofluorescent labeling of these cells with Iba-1 and imaging them on a confocal microscope. Then I take those images and calculate cell body size and branch filament length.

Figure 4: Microglia activation profile in the NTS based on morphological changes from the ramified to amoeboid-shape.